Polypharmacy Linked to Cognitive Decline in Newly Diagnosed Parkinson’s Patients, Study Finds
Written by |
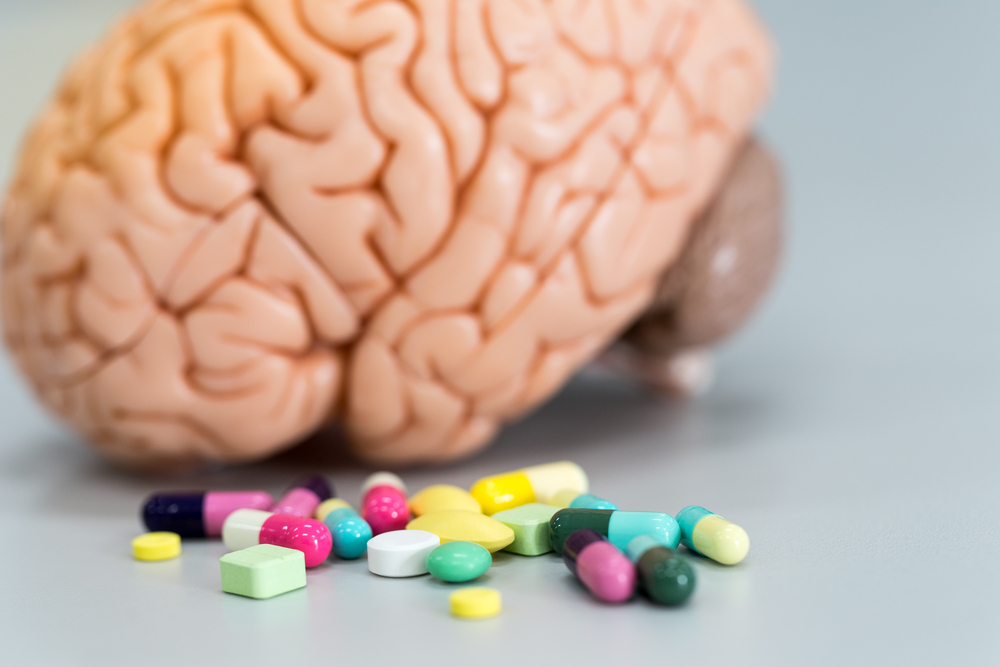
Taking several different medications at the same time to treat concurrent health conditions — known as polypharmacy — may be associated with cognitive decline in people newly diagnosed with Parkinson’s disease, according to a recent study.
Reducing the number of medications prescribed would be one option to minimize the potentially harmful effects of polypharmacy on patients’ cognitive abilities, the researchers said.
The study, “Polypharmacy Associated with Cognitive Decline in Newly Diagnosed Parkinson’s Disease: A Cross-Sectional Study,” was published in the journal Dementia and Geriatric Cognitive Disorders.
Polypharmacy — most commonly defined as taking five or more medications concurrently for different conditions — is an emerging concern, particularly for the elderly. It has been associated with falls, adverse medication events, and hospitalization, researchers say.
A previous study found that polypharmacy also is associated with cognitive impairment in older adults who live independently.
However, its effects on the cognitive function of newly diagnosed patients with Parkinson’s disease — a neurodegenerative disorder associated with cognitive impairments and, at later stages, dementia — are still unclear.
In this study, investigators from the University of Miyazaki in Japan set out to explore the possible association between polypharmacy and cognitive decline in people who were recently diagnosed with Parkinson’s.
The cross-sectional study enrolled 131 patients who had been consecutively hospitalized at the University of Miyazaki Hospital and were newly diagnosed with Parkinson’s. Participants were divided into two groups, depending on whether they met the criteria for polypharmacy — which was defined for this study as taking six or more medications to treat different health conditions.
Cognitive function was assessed in all study participants using the Mini-Mental State Examination (MMSE) and compared between the two groups. All comparisons were normalized for potential confounders, including age, sex, education and medical history.
Among the 131 patients (mean age 69.8 years, 46.6% male) enrolled in the study, 43 (32.8%) met the criteria for polypharmacy.
After performing data adjustments for possible confounders, researchers found that the individuals who met the polypharmacy criteria had significantly lower MMSE scores compared with those who did not (26.2 versus 27.7). These results were indicative of cognitive decline.
“This is the first study to demonstrate an association between polypharmacy and cognitive decline in patients with newly diagnosed PD [Parkinson’s disease], as well as in community-dwelling older adults,” or people living independently, the researchers said.
“Medication reduction might be a promising intervention to prevent the development of dementia in patients with early PD,” the investigators said.
“Further prospective studies are needed to confirm whether medication reduction in patients with newly diagnosed PD can improve cognitive function and prevent the development of dementia,” they added.


David C Read
This is me. Early PD, cirrhosis being treated. Gabapentin prescribed for nueropathy