My ‘TBM’ Tools for Parkinson’s Self-management
Written by |

Since being diagnosed with Parkinson’s disease (PD) in 2014, I’ve been on a quest to discover scientifically validated tools that will enable me to live better with this disabling disease. My name for this toolbox, my Parkinson’s self-management program, is TBM. “T” is for threshold management, “B” is for brain rewiring, and “M” is for mindful movement.
The tools and functions involved in my TBM practice are provided in the following table:
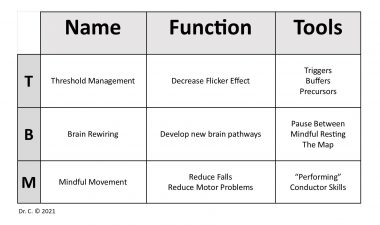
TBM functions and tools. (Courtesy of Dr. C)
The worst part of life with Parkinson’s are the ugly days when neither brain nor body work. I can’t succumb to the doom-and-gloom picture painted by professionals. There has to be a way to retrain my Parkinsonian brain.
For seven years, I’ve been in the trenches battling Parkinson’s, slowing the progression, and working out the details of TBM. There has been so little help in the way of brain rehabilitation for folks like me, until now. TBM helps me manage the disease and makes life more tolerable, even during the worst of times. It’s not a cure, but I wish I had these tools when diagnosed.
Previous columns described TBM components. I expect that TBM will need to be uniquely tailored to other PD patients to be effective. As researchers work out how to apply TBM to a broad population, there are likely to be some universal strategies helpful to implementing it. Following are several support steps.
Commitment
The first and most important step is commitment. I would love to say that using TBM is easy and fun, but putting it into daily practice is difficult. Relearning everything, including movements and inner reactions to the different flicker effects, is a full-time job requiring focused commitment every day.
PD challenges a patient’s ability to focus and carry out future intentions, often called executive functioning. The capacity to follow through on intent is consistently impaired in people with Parkinson’s, which is likely to have an impact on practicing TBM.
A 2015 research article published in the journal Frontiers in Human Neuroscience notes that “studies using both event-based paradigms, which require subjects to execute a delayed action at the occurrence of an environmental cue, and time-based tasks, which require subjects to execute a delayed action at the expiration of a certain time, document that PD patients perform significantly worse than healthy controls.”
TBM is about brain rewiring, and both patience and dogged persistence are needed to show up ready to do the work every day. Like getting the body in shape, the brain needs exercise. It’s the only way it will grow new neural pathways.
Much additional research is being done to understand these neural networks. A group of researchers studied Parkinson’s disease dementia and published their findings in the journal Brain in 2015. The abstract states that, “New treatments are slow in development because unlike the pathological process underlying the motor deficits of Parkinson’s disease, the neural mechanisms … are still poorly understood.”
With Parkinson’s, there is dysfunction in several neural networks. The abstract continues, “There is also growing recognition of the importance of cognitive rehabilitation therapies for managing dementias such as PDD. … Although the improvements seen were modest, this result … could be due to plastic effects on the underlying neural networks.”
Mindful exercise
Secondly, TBM works best with a body in shape. Doing core muscle workouts, such as boxing, tai chi, or yoga, for 10 hours a week can help with mindful movement. I build gardens, which involves lots of mindful shoveling and hauling. I use this exercise to counter the postural instability flicker. The Davis Phinney Foundation for Parkinson’s has a particularly good series on core strengthening techniques and their benefits.
A stable routine
Thirdly, TBM works best within a stable life routine, one without drama or stress. I’ve established a routine that fits my biorhythms. It’s not the same timetable most people use. Letting go of expectations that don’t fit is part of the program.
Self-awareness
My final TBM support step is to develop strong, accurate self-awareness. A review article published in the journal Parkinson’s Disease describes a review of self-management strategies used by PD patients. Authors found seven main themes: medication management, physical exercise, self-monitoring techniques, psychological strategies, maintaining independence, encouraging social engagement, and providing knowledge and information.
These are important, similar to the CHRONDI Creed developed in my book, “Possibilities with Parkinson’s: A Fresh Look.” TBM goes one step further in specifically retraining my Parkinsonian brain.
TBM isn’t easy, but it is effective in my life and offers hope when this ugly, progressive illness makes me run the gauntlet of suffering. TBM has changed my life from horrible to pretty good — most of the time.
***
Note: Parkinson’s News Today is strictly a news and information website about the disease. It does not provide medical advice, diagnosis or treatment. This content is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or another qualified health provider with any questions you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you have read on this website. The opinions expressed in this column are not those of Parkinson’s News Today or its parent company, Bionews, and are intended to spark discussion about issues pertaining to Parkinson’s disease.





Catherine
Thank you for this timely message and the added benefit of some new tools for my 'toolbox'! I have been living in denial regarding my deteriorating executive functioning for some time and feeling overwhelmed by my growing, self imposed, tasks-at-hand, What I do have working for me is dogged determination and a stubborn streak bar none to tackle my to-do list of both mental and physical tasks...like rehabbing an RV and finishing a second edition of a photography book I started around the time of my diagnosis (2015). Recognizing that the difficulties I am experiencing to stay on-task is part of the Stinkin'Parkinson's package gives me an explanation rather than a self-blaming excuse and is yet another lesson in patience and grace allowing for my 'slow' progress...but like my movements - said this tortoise, I will mindfully take it slow and steady and continue looking and moving forward. Much gratitude Dr C!
Sandra Ross
I have a question/comment re: the above articl, which I enjoyed very much. I've dealt with Chronic Fatigue Syndrome for over 30 years. A couple of years prior to being diagnosed with Parkinson's I noticed the fatigue was becoming worse, but something was different. The fatigue has become profound and it is difficult to maintain any routine. I've had severe reactions to medication'medications (I'm 77) and am at a loss.
William Palmer
A few times when I have felt on the edge of losing hope, I read one of your articles, Dr. C. They renew my hope. They help me a great deal. Thank you.
LM Kerrigan
Great article. I'm very much interested in learning more about TBM. Are the "tools and functions" laid out in a single document, guide or book, or are they contained in the recommended readings referred to in this article? Or am I just missing something? Thanks.
jennie jo flannery
i am 77 year
sold and also suffer with fatiigue. I was diagnosed in 2016 April 15th. THIS i very hard for me also. I wish i had
the answer.Also, this effects my eyes. At times when I am eating, my vision becomes blurry.
Judy Allen
I was diagnosed with Parkinson this year in 2022 and am 74 yrs. old. This is very depressing to have and am trying to fight it with essential oils. I have a friend that is a retired critical nurse and she nursed her mom who had cancer and she is now in remission due to the oils. I am using her formula for Parkinson but at times I forget to take it, these oils are expensive. I only have the tremors which drives me nuts. I am a professional quilter and these tremors are really taking a toll on me. I enjoy reading these articles that are posted and looking forward to learning from them.