Older Parkinson’s Patients Often Wrongly Given Antipsychotics, Study Says
Written by |
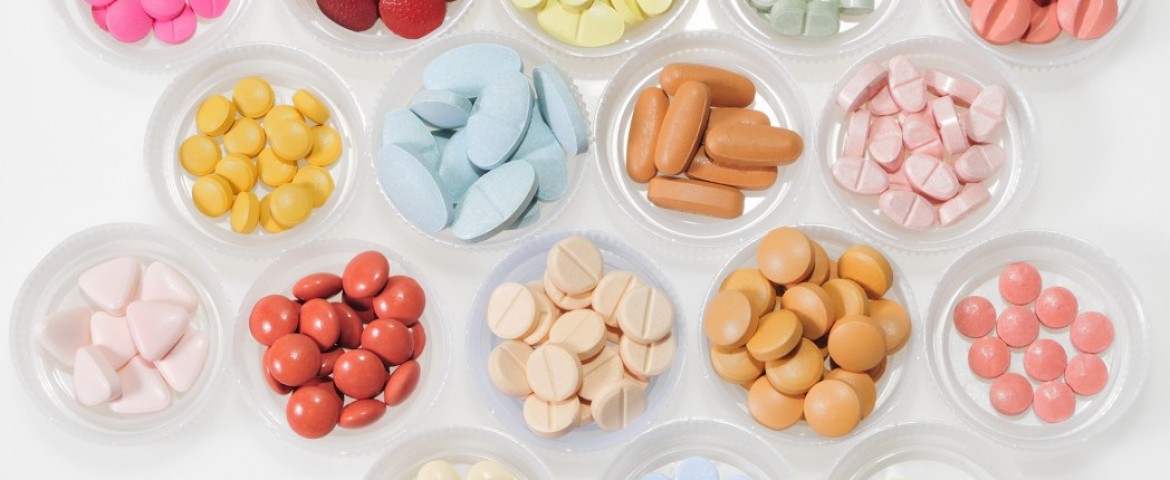
More than one-third of older people with Parkinson’s disease in long-term care who experienced therapy-related psychosis were prescribed antipsychotic medications considered inappropriate under current guidelines, a study found.
Those with dementia or using antidepressants were more likely to be given these medicines.
Concerted efforts are needed to curb the use of inappropriate antipsychotics, which may worsen Parkinsonian symptoms, the researchers said.
The study, “Use of Atypical Antipsychotics in Long-Term Care Residents with Parkinson’s Disease and Comorbid Depression,” was published in the journal Dove Press: Drug, Healthcare and Patient Safety.
The use of dopamine replacement therapies such as levodopa can alleviate movement-related symptoms in people with Parkinson’s, but can also bring about visual hallucinations or delusions known as psychosis.
Although the use of antipsychotics is typically recommended for psychotic symptoms, according to the 2015 American Geriatrics Society (AGS) Beers criteria, some antipsychotics are inappropriate for people with Parkinson’s because they increase the risk of worsening Parkinsonian symptoms.
Antipsychotics deemed inappropriate under the guidelines include asenapine (brand name Saphris, among others), Rexulti (brexpiprazole), Fanapt (iloperidone), Latuda (lurasidone), Zyprexa (olanzapine), Invega (paliperidone), Risperdal (risperidone), and Geodon (ziprasidone).
As few studies have examined the use of inappropriate, atypical antipsychotics in older patients with Parkinson’s, a team of researchers based at the University of Houston designed a study to evaluate the extent of inappropriate antipsychotic use in Parkinson’s patients living in nursing homes.
Atypical antipsychotics are those that are less likely than traditional antipsychotics to cause certain side effects, including Parkinsonian symptoms.
The team analyzed the medical records of patients who experienced depression as a co-condition. Using a 12-month baseline and 24-month follow-up, they examined the inappropriate use of atypical antipsychotics as well as the use of appropriate atypical antipsychotics, including aripiprazole (brand name Abilify, among others), clozapine (Clozaril, among others), and Seroquel (quetiapine).
The mean age of the study group was over 80.
Of the 76,294 Parkinson’s patients selected for review, 13,352 (17.5%) were given atypical antipsychotics, and the rate of inappropriate use among atypical antipsychotic users was 36.32% (4,849 patients).
Those who were less likely to be given inappropriate antipsychotics were highly educated, married, and living in the Northeast.
Older patients were more likely to be given inappropriate antipsychotics.
Those with dementia or chronic obstructive pulmonary disease (COPD) were more likely to be given inappropriate antipsychotics, as were those treated with the antidepressants selective serotonin reuptake inhibitors (SSRIs) or serotonin–norepinephrine reuptake inhibitors (SNRIs).
In contrast, patients who were taking the dopamine agonist levodopa were less likely to receive inappropriate antipsychotics. Also less likely to receive these medicines were those who were prescribed other dopamine agonists, catechol-o-methyltransferase (COMT) inhibitors such as Comtan (entacapone) and Tasmar (tolcapone); monoamine oxidase (MAO) inhibitors type B such as selegiline (Eldepryl, Zelapar); or Gocovri (amantadine).
“The incidence rate of inappropriate atypical antipsychotic use was relatively high, as more than one-third of PD patients received inappropriate agents among those who were treated with atypical antipsychotics in this study,” the researchers wrote.
“Further research is warranted to evaluate rates and patterns of antipsychotic use after the implementation of new guidelines for PD psychosis,” they said.

Leave a comment
Fill in the required fields to post. Your email address will not be published.