High Exposure to Antibiotics May Increase Risk of Parkinson’s, Study Suggests
Written by |
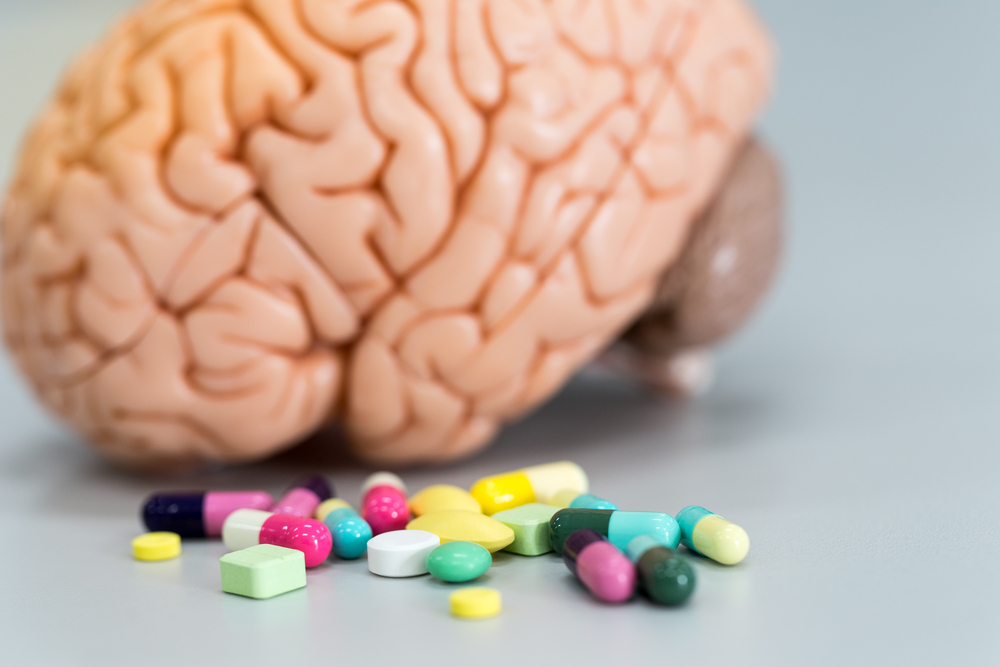
High exposure to oral broad-spectrum antibiotics and those that kill anaerobic bacteria and fungi is associated with a high risk of Parkinson’s disease within the next decade or more, a study finds.
The findings were reported in the study “Antibiotic Exposure and Risk of Parkinson’s Disease in Finland: A Nationwide Case-Control Study,” which was published in Movement Disorders.
Excessive exposure to antibiotics may change gut bacteria composition, which in turn is associated with an increased risk of several psychiatric disorders, Crohn’s disease, and colorectal cancer. Now scientists are also starting to investigate the possible link between antibiotic use and Parkinson’s.
“The link between antibiotic exposure and Parkinson’s disease fits the current view that in a significant proportion of patients the pathology of Parkinson’s may originate in the gut, possibly related to microbial changes, years before the onset of typical Parkinson motor symptoms such as slowness, muscle stiffness and shaking of the extremities,” Filip Scheperjans, MD, PhD, principal investigator of the study and neurologist at Helsinki University Hospital, said in a press release.
“It was known that the bacterial composition of the intestine in Parkinson’s patients is abnormal, but the cause is unclear. Our results suggest that some commonly used antibiotics, which are known to strongly influence the gut microbiota, could be a predisposing factor,” he said.
To further explore the possible association between high exposure to antibiotics and the onset of Parkinson’s, investigators from Helsinki University Hospital in Finland carried out a nationwide case-control study to compare antibiotic exposure in a large group of people with and without Parkinson’s.
The study included data from 13,976 people who had been diagnosed with Parkinson’s in Finland between 1998 and 2014, and 40,697 people who were the same age and sex, and from the same place of residence, but who did not have the disorder (controls). Information from patients and controls was obtained from national registries.
Antibiotic exposure was estimated based on data about purchases of oral antibiotics and was analyzed in three different time-points: one to five years, five to 10 years, and 10 to 15 years before the onset of Parkinson’s. In their analyses, investigators also looked at antibiotic exposure after grouping medications in different categories (e.g. by chemical structure, antimicrobial spectrum, and mechanism of action).
“During the course of follow-up, 84.9% of [Parkinson’s disease] patients and 83.6% of controls had purchased at least 1 antibacterial course. Penicillins were purchased most frequently, constituting 22.8% of all purchases,” the researchers wrote.
On average, people with Parkinson’s purchased more antibiotic courses than controls (6.32 versus 6.25), but the controls were hospitalized more often due to bacterial infections (0.19 versus 0.16).
The strongest connection to Parkinson’s was found for exposure to oral macrolides and lincosamides, two different classes of antibiotics that target different types of bacteria and work by preventing bacteria from producing the proteins they need to survive.
Further analyses showed that exposure to broad-spectrum antibiotics such as tetracyclines, and those that specifically target anaerobic bacteria, were associated with an increased risk of Parkinson’s disease within 10 to 15 years.
In addition, other types of antibiotics, such as sulfonamides and trimethoprim, and antifungal medications, were found to be associated with an increased risk of the disease within one to five years.
“Although no conclusions regarding causality can be made, it is plausible that oral antibiotic exposure is one factor that makes the gastrointestinal tract more susceptible to [Parkinson’s] pathology,” increasing the risk of getting the disease, the researchers said.
“Our findings demand confirmation in different cohorts. However, if confirmed in future studies, a connection between commonly prescribed oral antibiotics and neurodegeneration could have major implications for prescribing practices and public health,” they added.

Leave a comment
Fill in the required fields to post. Your email address will not be published.