Managing Parkinson’s Disease Is a Full-time Job
“Dealing with a diagnosis of Parkinson’s is not easy and there is no one, single technique that will ease the pain and no magic pill that will miraculously enable you to cope with it.” — John Baxter
Parkinson’s treatment is a lifelong commitment that involves much more than just taking a pill.
When I was first diagnosed in 2015, I naively thought that all I would have to do is take Sinemet (carbidopa/levodopa) to make me feel better. Over time, and as my disease progressed, I realized that no one-size-fits-all remedy exists to resolve all of my symptoms. A combination of therapies, exercise, medications, and supplements is required.
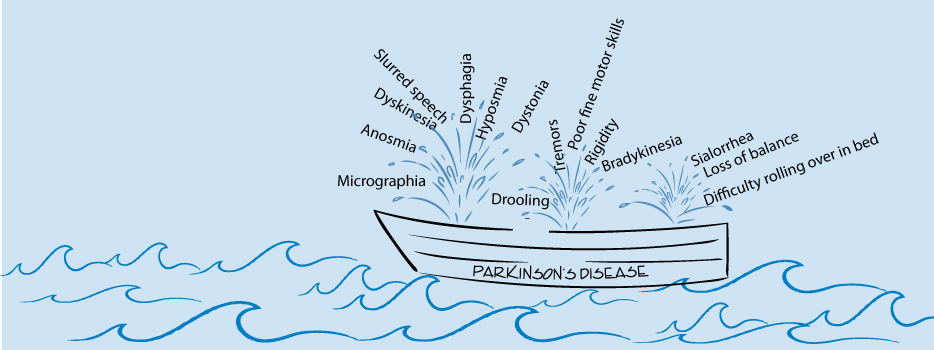
As my naturopathic doctor says, Parkinson’s is like a boat with many holes that need multiple plugs to fill them. Because Parkinson’s has so many potential symptoms, plugging each of the boat’s holes can be like an unsalaried full-time job, plus overtime.
Although I can think of better activities to do in retirement, I am thankful that I no longer work so that I can devote my time to improving my quality of life.
And people wonder what I do with all of my time now that I am retired!
Therapies
Multiple medical professionals have told me I have to invest less than 30 minutes of my day to see improvement in a particular symptom. However, if we multiply those 30 minutes by the various symptoms, the hours in the day start to disappear quickly.
Physical therapy sessions for balance and core strengthening, which are important to prevent falls, must be scheduled. Occupational therapy, such as picking marbles out of rice, helps to improve my fine motor skills. Speech therapy, such as the Lee Silverman Voice Treatment, or LSVT, is needed to help improve my slurred speech and voice projection.
Plus, there is no shortage of homework to do for these therapies. Exercises involving swallowing, balance, and other fine motor skills must be performed daily. Additionally, there is sniff training using essential oils to improve my failing sense of smell. Then there are handwriting exercises to improve my illegible writing.
It’s essential for people with Parkinson’s to keep moving, so I also incorporate regular fitness training into my week, such as walking, cardio machine workouts, and weight workouts.
Attendance at Parkinson’s support group sessions is critical for socialization.
And I plan to add meditation for my mental health.
Prescription medications
Medications mainly address the movement disorders that are characteristic of this disease, such as bradykinesia, tremors, and dystonia. I take carbidopa/levodopa four times a day and apply a Neupro (rotigotine) patch daily. I also take selegiline twice a day because some studies have shown it potentially can slow disease progression.
I also take Nourianz (istradefylline), which is used to improve the efficacy of carbidopa/levodopa by reducing and shortening the off periods a patient may experience. I never thought I would see the day when I take one medication to help another medication work better.
Supplements
I take multiple supplements recommended by my naturopath doctor, including vitamin D, fish oil, CoQ10, and glutathione. Based on her research, my naturopath doctor has found that people with Parkinson’s typically are on the low end of the nutrients that these supplements address.
I can’t be certain whether these supplements are helping my symptoms and slowing progression. Therefore, I will continue to take them in case I might feel worse without them.
Wait, there’s more
On some days, I’ll spend many hours online, researching the latest and greatest “cures” and remedies. I also spend a lot of time online looking for products that improve quality of life, such as satin pajamas and bedsheets to ease the difficulty of rolling over in bed, or the best pen to help improve my handwriting.
Other Parkinson’s symptoms that don’t affect me, or that affect me only slightly, such as incontinence, cognitive loss, sleep issues, and depression, have their own individual “plugs,” or remedies.
Fatigue and apathy are two of my most debilitating symptoms. Finding a feasible way to plug these holes in the Parkinson’s boat can at times be an exercise in futility. It is a vicious circle: I need to move and exercise to feel better, yet fatigue and apathy put up constant roadblocks.
Feeling overwhelmed
Before my Parkinson’s diagnosis, I chose to exercise five to seven days per week because I enjoyed it. Now, it is such a struggle to get motivated to exercise, attend my therapy sessions, and complete my therapy homework. Sometimes, I just want to go back to bed.
However, although I am the captain of my ship, I will not go down with it!
I just have to keep bailing so that I don’t sink!
“I often think I can’t do this anymore but then I realize what choice do I have?” — Justin Blaney
***
Note: Parkinson’s News Today is strictly a news and information website about the disease. It does not provide medical advice, diagnosis, or treatment. This content is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or another qualified health provider with any questions you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you have read on this website. The opinions expressed in this column are not those of Parkinson’s News Today or its parent company, Bionews Services, and are intended to spark discussion about issues pertaining to Parkinson’s disease.







Best Ketamine Clinics
Cool, this article improved my mood. The author is a very positive person! My mother has this disease and I surf the Internet almost every night in search of a new solution. I believe that one day all diseases can be cured, so I constantly check this. I completely agree with the author's idea about the boat. I try my best to help my mother, because apart from constant therapy and the pills prescribed by the doctor, we do a lot more. We try to start every morning with a meditation. Mom says that after the meditation, it becomes a little easier for her to start the morning. We also drink vitamins and eat right. I wish the author good and strong health and that he would never lose his optimism!))
thank you for your comment. Meditation is something I am going to add to my list
Denise Crouse
My good friend is a huge advocate for meditation and I’ve seen it help me tremendously within a few days. There are a few apps that are helpful if you need a ‘jump start’ ?
Nels Johnson
This was very helpful, as my journey so far has been quite similar. I recently replaced my desk with a "standing desk" so I can use my computer during off periods when I need to keep my arms and legs moving. I am also planning to invest in a Theracycle--expensive but I believe it will substantially improve quality of life, slow down Sinemet dosage escalation, and help with fatigue and balance issues.
Hi Nels, thanks for your feedback. Sounds like you have a good plan. The Thera cycle seems like a good thing and if I had the room, I would love to try it. If u do get one, it would be great if you could post your theracycle experience on our Parkinson’s forum
John Humphreys
Spot on analysis. I am in violent agreement with everything you said!
Thank you John. I appreciate your comments1
Sandy Stahl
I concur my dear friend and Warrior. - Sandy Stahl
Charaf
Bonjour, un article vivifiant. Cependant, je pense que l'augmentation des doses de la levodopa est inversement proportionnelle aux facteurs de résilience: activités physiques régulieres et soutenues, alimentation ciblée, méditation, herbes etc.
translation:
Hello, an invigorating article. However, I think that the increase in the doses of levodopa is inversely proportional to the factors of resilience: regular and sustained physical activities, targeted diet, meditation, herbs etc.
Thank you Charaf for sharing your thoughts!
Allen Perez
Querida Jean, me levantó el ánimo leer tu artículo. Siento que debo ser realista a la vez que activo y creativo. Empiezo a practicar meditación y un poquito de baile. Veo que es importante moverme y sentir alegría. Seguiré motivando mi corazón con las bellezas que la vida me ofrezca. Creo que ya soy un artista de la existencia y la esperanza. Muchas gracias...
TRANSLATION:
Dear Jean, I was encouraged to read your article. I feel like I have to be realistic as well as active and creative. I start to practice meditation and a little dance. I see that it is important to move and feel joy. I will continue to motivate my heart with the beauties that life offers me. I think that I am already an artist of existence and hope. Thanks a lot…
Thank YOU Allen for sharing your thoughts!
Richard Malmsheimer
Thank you for this reminder.
Richard, I think it bears repeating. thanks for your comment
Richard Malmsheimer
My reminder--helpful some days: I'll do as much as I can, as well as I can, for as long as I can. And when I can't, I'll DO something else.
Richard, that is a great approach! Attitude is so important.
Amir Delfarah
My Dad diagnosed to Parkinson on March 2020 when his tremors become more serious. His tremor in chin area is really hurting him as he can not sleep or even eat properly. Dad and his partner lives in Iran and I’m living in Australia, In this unprecedented Covid situation, All I can do is just being with him and keep close contact with FaceTiming so he don’t feel alone.
Thankfully , my Older sister lives very close to Dad’s place and she is a nurse .. so she is taking good care of him .
I have heard of DPS surgery that can help easing Parkinson symptoms dramatically which I’m so excited about. Can you please advise your thoughts on DPS surgery?
Hi Amir, I am sorry Covid is preventing you from seeing your Dad. I think you are referring to DBS surgery. Your Dad's doctor would be the best person to determine if DBS is right for your dad. Here are some links for you to reference to give you some background.
https://www.michaeljfox.org/news/deep-brain-stimulation
https://www.parkinson.org/Understanding-Parkinsons/Treatment/Surgical-Treatment-Options/Deep-Brain-Stimulation
https://davisphinneyfoundation.org/?s=dbs
Emily
Thank you for this article and for the idea of managing Parkinson's as a "lifelong commitment." There are so many different symptoms people living with Parkinson's face, and there isn't a one-size-fits-all approach to managing the disease. For some people, research shows a positive link between Parkinson's and regular exercise, as I learned in this article: https://specialtycareservices.com/exercise-and-parkinsons/.
Emily Thnk you for your comment. Exercise is key, however the cruelty of PD for me is that it robs me of my motivation to exercise . I am so fatigued and muscles getting weaker even though I continue my weight workouts. I used to be an athlete before PD so I still have ability to go on autopilot and push myself. Yes, continued movement is key,,,